DEMOGRAPHICS
Name: C.B.
Age: 62 years old
Case/Type: Heavy/Type II
ASSESSMENT
This patient had his last medical exam in March of 2019. He is allergic to pork and pineapple. He was never hospitalized because of it, but he has experienced anaphylaxis in the past. C.B. had a hip operation in 2001. He was scheduled for back surgery on April 28th, 2019, but it was postponed until July of 2019 due to issues with hospital administrative procedures (paperwork not being filed). This patient suffers from life-long depression. He stated that he was abused as a child. He has recurring sinus trouble (stuffy nose and congestion). The patient also stated that he has severe-stage OSA. He clenches at night to prevent snoring. C.B. was recommended to use a CPAP machine after he had his last sleep test approximately two and a half years ago. He thought that his symptoms have since improved, so he stopped using it, but now his snoring has returned. C.B. exhibits signs of mouth breathing (chronic dry mouth, chapped lips, localized marginal gingivitis).
C.B.’s initial blood pressure reading was 172/122 and his pulse was 76 beats per minute. The second blood pressure reading was 169/104 and his pulse was 73 beats per minute.
C.B. does not drink alcohol but he smokes about 7-10 cigarettes per day for the past 40 years.
C.B. did not require any premedication for dental treatment.
C.B. takes Albuterol 90 mcg for chronic asthma which he has had since 2001.
Albuterol (Ventolin HFA) is a prescription drug used to treat asthma and bronchospasm.
ORAL PATHOLOGY (Extraoral and Intraoral findings)
C.B.’s extraoral exam produced “popping” on the right side of his TMJ but he stated that he does not experience any pain from it. He stated that he does clench his teeth at night. Enlarged tonsils (obstructed airway) and an enlarged, coated tongue were found during his intraoral exam. Additionally, the patient had slightly fibrotic tissue on his lower right, upper middle and upper left lip (from biting). The patient also had hyperkeratinized tissue on the right buccal mucosa from biting and sucking his cheeks due to the absence of teeth #s 1, 2, 4, 5 and 30. C.B. also had hyperkeratinization on the left and right side of his tongue.
DENTITION
C.B.’s class of occlusion was Class I with 5% overbite and 2 mm overjet.
C.B. had occlusal amalgam restorations on teeth #s 12, 13, 17, 21, 28 and 29, a disto-occlusal amalgam restoration on tooth #15, an occlusal-buccal-lingual amalgam restoration on tooth #3, and an occlusal-buccal amalgam on tooth #18. He was missing teeth #s 1, 2, 4, 5, 14, 16, 19, 20 and 30.
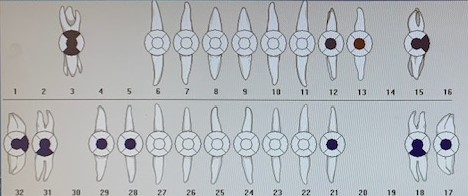
C.B. had caries present on tooth #13O.
PERIODONTAL
C.B. was classified as a Heavy Case, Type II. This patient’s probing depths were between 3-4 mm. He had minimal bleeding upon probing.

ORAL HYGIENE
C.B.’s initial plaque score was 2.0 (poor). At the time of his subsequent appointment, the plaque index score was also 2.0 (poor).
C.B. had generalized staining, heavy interproximal, facial and lingual subgingival calculus deposits present on the posterior surfaces and the facial/lingual anterior teeth.
C.B. reported brushing one time per day in the morning with an electric toothbrush. He also stated that he uses floss picks periodically throughout the day and ACT mouthwash one time per day. I reviewed the appropriate electric toothbrushing technique with this patient and instructed him to focus on posterior areas. The patient answered positively to a sleep apnea symptom questionnaire. I advised the patient to practice nasal breathing and to be aware of open-mouth posture. I also provided the patient with a referral for a sleep test.
At the patient’s next visit, I demonstrated flossing with waxed dental floss and the patient practiced the technique.
RADIOGRAPHS
C.B. had an FMS done at a dental clinic in March of 2018. He required bitewing radiographs to assess the level of bone loss in the intended Arestin placement sites.

ARESTIN PLACEMENT
I placed Arestin (minocycline HCl microspheres 1 mg) in the following sites: #17MB, #18DB, #31DB, #32ML and #32MB on March 28th, 2019.

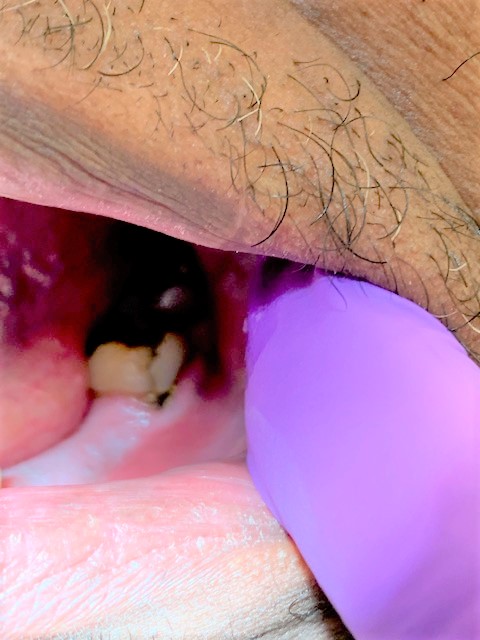
ARESTIN EVALUATION
C.B. returned for a post-Arestin placement evaluation on May 17th, 2019.The following graph shows the reduction in pocket depths in the sites that were treated with Arestin.
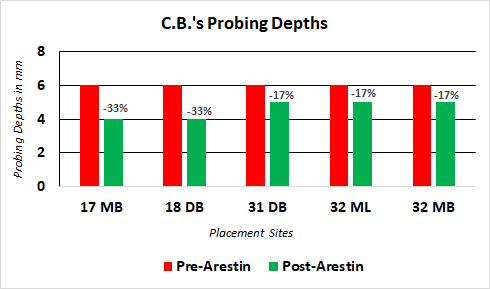
A



