My patient Mr. J is a 30 year old Asian male. His vitals were 118/63 with a pulse of 70. He is a non-drinker but he is ASA II due to smoking of electronic cigarettes and mild seasonal allergies. He is taking Claritin 10mg/day for his seasonal allergies. FMS was recommended to this patient because his last radiographs were taken on 2015.
Few things were noted during extraoral and intraoral examinations. Acne was predominantly present on patient’s right face. Due to the acne, his right side of the preauricular skin, was dry. Also, fissures were present on the left lateral commissure due to his dry lips.
During intraoral examination, enlargement of patient’s right tonsil, maxillary torus, coated tongue and and linea alba bilaterally were noted in the clinical note.
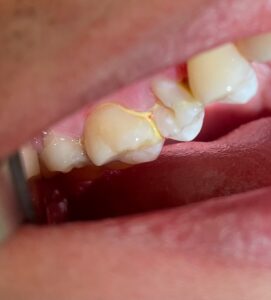
His occlusion was class Ill bilaterally. He had a cross bite with an overjet, and 10% overbite. #1, #17, #32 were not clinically present. He still had his primary tooth “A” that was not exfoliated, and interestingly, it was connected to #4 by resin filling. #10 and #21 were tilted lingually, and #20 was tilted towards the buccal.
He also had localized attrition on maxillary and mandibular anteriors.
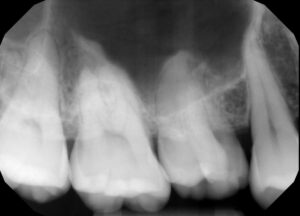
Primary tooth connected to #4 was captured in the premolar PA shot.
His gingival was pink, localized stippled, generalized red GM, puffy. He had generalized moderate marginal gingival inflammation. He also had generalized BOP with generalized 4-7 mm depth on posteriors. Generalized mandibular anterior supra/subgingival calculus and localized subgingival calculus on maxilla anteriors were found.
For his treatment plan, FMS, full mouth scaling, engine polish, application of 5% sodium fluoride varnish were planned and it was discussed with the patient.
FMS at 70 kVp and 7 mA was exposed during his second visit. Radiographs revealed localized 10%~15% of bone-loss on maxillary posteriors and impaction of #17 and #32. Generalized calculus were also noted, but there were no carious lesions.
His plaque index score came out as 1.3; fair. The biofilms were mostly present on cervical third and interproximally. By that, demonstration of floss was conducted for the patient education.
With hand scalers and ultrasonic scalers, full mouth scaling was conducted with 3 visits.
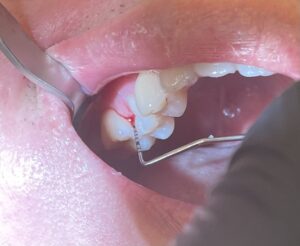
During the re-evaluation on his second visit, 6mm of pocket depth was still present on #3-MB. With the consent of my patient, we decided to place Arestin®. Post-op instruction, active ingredient, returning for re-evaluation were fully reviewed with the patient. All of the consent forms were scanned into e-chart.
Patient returned for his re-evaluation of the Arestin® site, #3-MB, after a month of placement. Depth of #3 MB was re-probed, and the measurement came out as 5mm.