Case Studies
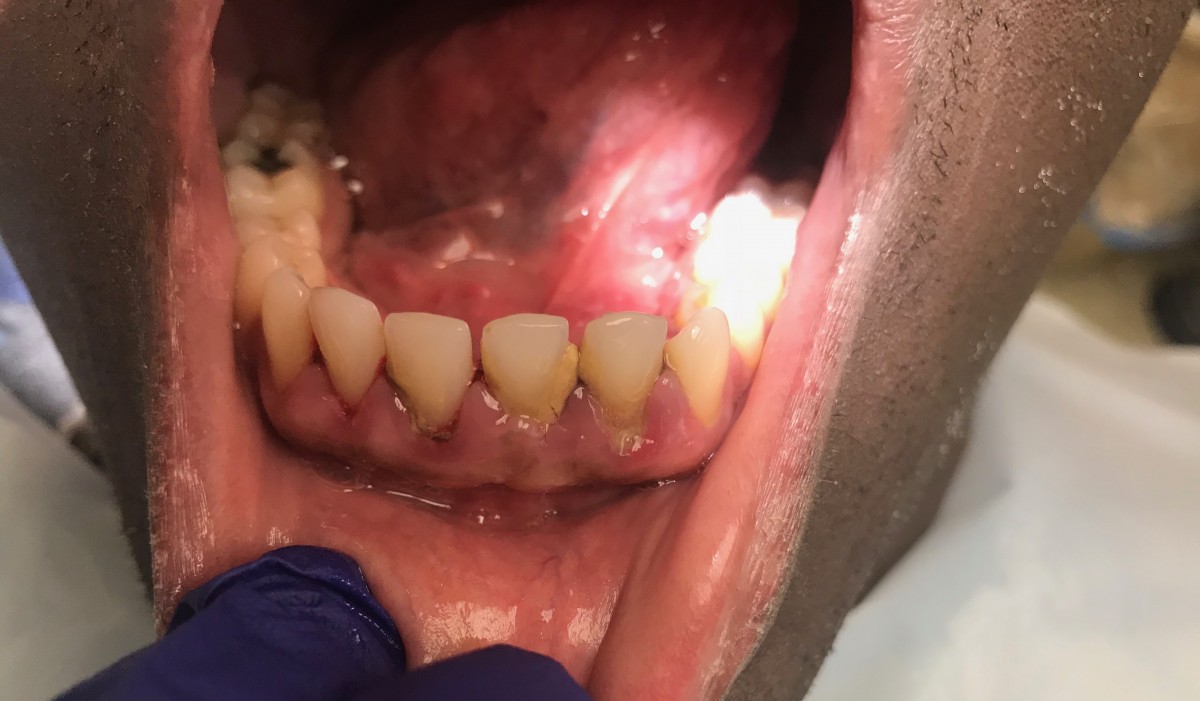
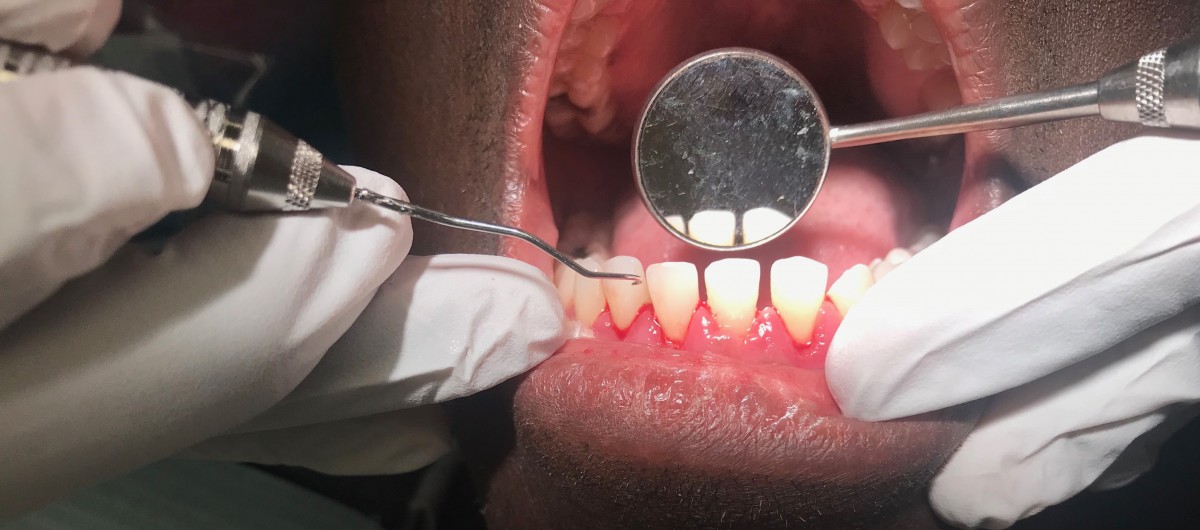
Case #1 and #2: The following are before and after images of two patients in their mid-20s with similar cases. Both presented for their first dental visit and have no previous dental experience. Both patients are ASA II due to their history of smoking for over 10 years. A complete assessment was done which included E/O, I/O exam, dental assessment, full mouth probe exam and a FMS. They had generalized 4-6 mm pockets and radiographic evidence of early bone loss. A complete debridement was done with pain management techniques such as, infiltration and Oraqix, to ensure the patients had a comfortable first time dental experience. Emphasis was given to educating the patients about smoking cessation and proper oral hygiene instructions.
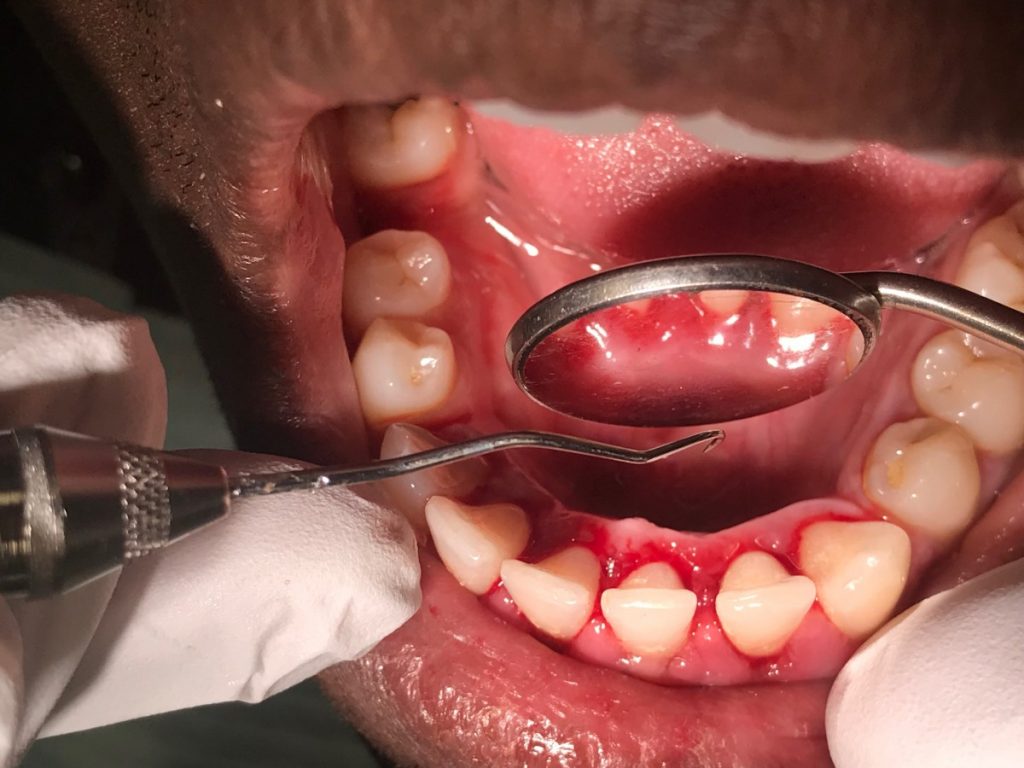
Case #3: This 58-year-old patient is diabetic and presented for a cleaning after 5 years. The patient had generalized 6-7 mm pockets, moderate bleeding upon probing, and moderate inflammation along the gingival margin. The patient’s A1C level during this time was a 7. His oral hygiene condition was below optimal. A FMS revealed the patient had generalized horizontal and vertical bone loss as well as a radiolucency under the abutment teeth in the mandibular anterior bridge. A complete debridement was done along with emphasis on educating the patient about home care. His plaque index score during the second visit was 1.2 which was an improvement from his first visit in which was the score of 1.8.
Case #4: Patient had generalized 5-6 mm pocket depths, severe bleeding upon probing, and severe inflammation. Radiographic findings revealed early signs of generalized bone loss. One week after complete debridement, the patient was given Arestin treatment in 8 sites with the deepest probe readings.
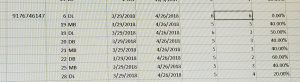
The log above was used to measure the percentage of change in the patient’s pocket depth 4 weeks after Arestin treatment. There was a reduction in pocket depths after 4 weeks.